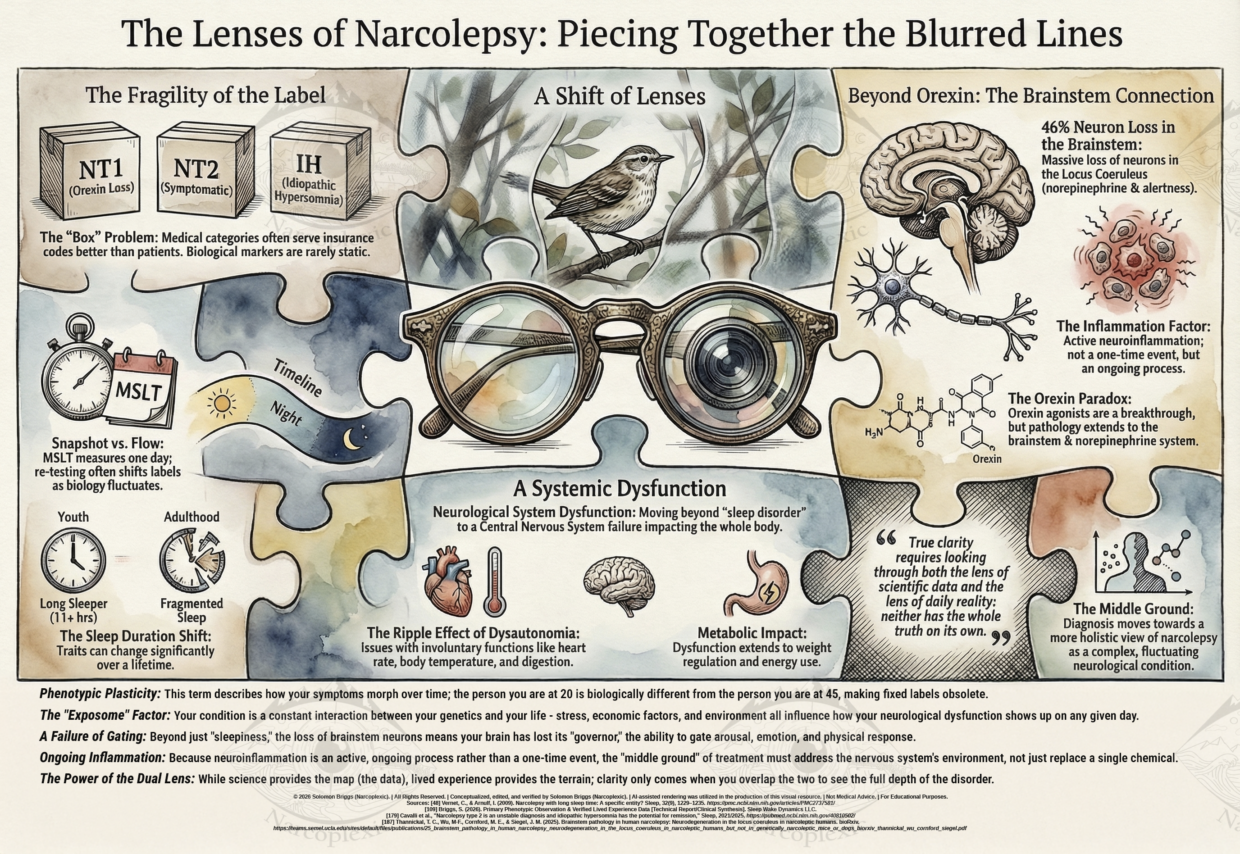
For a long time, the medical world has tried to keep things simple. If you have narcolepsy, they want to put you in a specific box. If you lose Orexin, you’re Type 1. If you don’t, but you still fall asleep, you’re Type 2. If your test results are slightly different, they call it Idiopathic Hypersomnia (IH).
But for people actually living with this, those boxes don’t always work. The symptoms don’t stay in one place, and the science is finally starting to show why.
The Problem with a One-Day Test
Right now, a diagnosis depends almost entirely on the MSLT (Multiple Sleep Latency Test). It’s a test that measures one single day of your life in a lab. The problem is that a person’s biology isn’t a static, unmoving thing. It changes.
Research has shown that when patients are re-tested later, their “label” often shifts. Someone might look like they have Type 2 Narcolepsy one year and IH the next. This isn’t because they have a different disease; it’s because the test itself is an unreliable snapshot of a condition that fluctuates.
- Changing Symptoms: It is possible for someone to be a “Long Sleeper” (sleeping 11+ hours) when they are younger and then deal with the fragmented, broken nighttime sleep of a typical narcoleptic as they get older.
- The Cataplexy Shift: Cataplexy isn’t always a “yes or no” thing that stays the same forever. For some, it can show up, disappear, or change in how it feels decades after they first started getting sleepy.
- Lifestyle and Environment: Factors like age, stress, and even your physical environment can change how the symptoms show up on a test.
The Gap Between Science and Lived Experience
When it comes to something like cataplexy, there is often a large gap between the science and the lived experience. It is like trying to focus a camera on a bird in the distance—there are branches in between the lens and the bird that cause the camera to lose and bounce focus.
Sometimes, the science gets so excited about a specific discovery that the actual lived experience of the patient ends up completely out of the frame. Other times, the people living with the condition are so close to it that they might not recognize a pattern or a biological fact that the science is finally bringing into focus.
Neither perspective has the whole truth on its own. We need a shift of lenses from time to time. Without both the scientific data and the reality of the daily experience, we won’t ever have actual clarity on the real depths of what is at play.
It’s More Than Just a “Sleep Disorder”
Calling this a “sleep disorder” doesn’t cover the full picture. It is a Neurological System Dysfunction. It’s a problem with the Central Nervous System that affects almost every part of the body.
When the part of the brain that regulates “arousal” (being awake and alert) isn’t working right, it ripples outward. It leads to Dysautonomia, which is when the involuntary parts of your nervous system struggle to do their job. This is why people with narcolepsy often deal with:
- Fragmented Night Sleep: Being unable to stay awake during the day, but unable to stay asleep at night.
- Metabolic Issues: Problems with weight and how the body uses energy.
- Autonomic Problems: Troubles with heart rate, body temperature, and digestion.
The Orexin Paradox: New Research from UCLA
There is a lot of talk right now about Orexin Agonists—new drugs designed to replace the Orexin that people with Type 1 Narcolepsy are missing. While these will be a big help for many, they might not be the whole answer.
Dr. Jerome Siegel’s team at UCLA has found that human narcolepsy involves more than just missing Orexin. Their research shows:
- Massive Cell Loss in the Brainstem: There is a 46% loss of neurons in the Locus Coeruleus, which is the area of the brain responsible for norepinephrine and general alertness.
- Ongoing Inflammation: They found evidence of active neuroinflammation in the brain. This suggests the condition isn’t just a one-time event where cells die, but a process that can change over time.
Moving Toward a Middle Ground
In the next ten years, the way doctors look at these rigid categories will likely change. The labels like NT1, NT2, and IH exist mostly for insurance codes and medical filing. They don’t always match the human experience.
The reality seems to be a “middle ground.” Narcolepsy is a complex, fluctuating neurological condition. It involves Orexin, but it also involves the brainstem, inflammation, and how our bodies react to the world around us. It is a lot more than just being tired.
Sources
- Thannickal, Siegel, et al. (2025/2026): Brainstem pathology in human narcolepsy teams.semel.ucla.edu/sleep-research
- Bassetti, C. L., Lammers, G. J., et al. (2025): Narcolepsy type 2 is an unstable diagnosis and idiopathic hypersomnia has the potential for remission: observations from the Bern Sleep–Wake Registry.
- Vernet & Arnulf (2009): Narcolepsy with Long Sleep Time: A Specific Entity?
Disclaimer: The information provided in this article is intended for informational and educational purposes only. Seek a qualified medical professional with expertise in Narcolepsy for diagnosis or treatment. I am not a medical professional.
Created by: Solomon Briggs
(aka Narcoplexic)
March 8th, 2026
The Lenses of Narcolepsy: Science, Lived Experience, and the Blurred Lines in Between © 2026 by Solomon Briggs is licensed under CC BY-NC 4.0
To view a copy of this license, visit https://creativecommons.org/licenses/by-nc/4.0/
“You may use this tool for non-commercial purposes, but must credit Solomon Briggs.”